Daten 2019 en
Data of the NRZMHi for Haemophilus influenzae 2019
1. Introduction
The tasks of the National Reference Laboratory for Meningococci and Haemophilus influenzae (NRZMHi) assigned by the Robert Koch Institute for the surveillance of invasive Haemophilus influenzae disease include serotyping of clinical isolates from blood or cerebrospinal fluid (CSF) and the detection of antibiotic resistance against β-lactam antibiotics.
In 2019, all in all 865 submissions were analyzed including bacterial isolates from 737 patients with invasive infections. The NRZMHi could confirm the diagnosis Haemophilus influenzae in 728 cases with invasive disease. In two cases H. parainfluenzae from blood was detected. Furthermore, seven H. influenzae isolates derived from primarily sterile sites other than blood or CSF. These cases do not meet the criteria of the reference definition for a notifiable invasive infection. In 699 invasive cases, H. influenzae was isolated from blood, 29 from cerebrospinal fluid (CSF) only. Detection of H. influenzae from these materials must be notified according to the German Infection Protection Act (IfSG).
In 2019, the statutory notification system registered 954 invasive H. influenzae infections. Since the NRZMHi transmits all laboratory results to the local health authorities in charge, the coverage of the laboratory surveillance can be estimated based on these data. Thus, a coverage of 76% can be assumed for 2019.
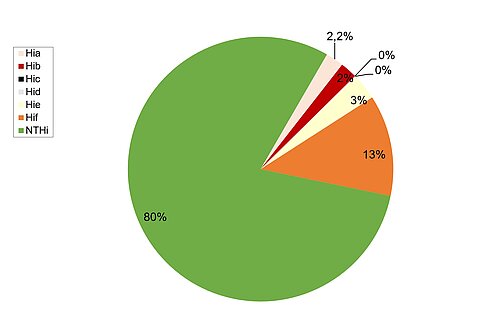
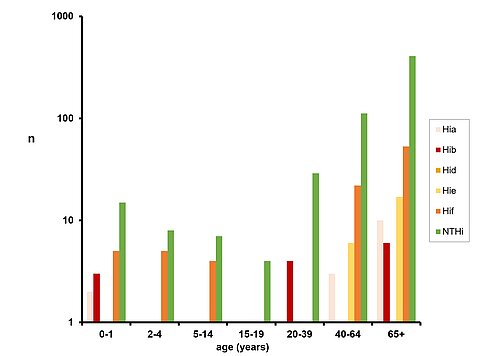
As in previous years, the majority of blood or CSF isolates were non-typeable H. influenzae (NTHi, 583 isolates, 80 %), followed by Hif as the most frequent capsular serotype (90 cases; 12 %). Hie showed third highest frequency among the serotypes (23 cases each; 3 %). Interestingly, this year, the previously rare serotype a (16 cases, 2 %) was as frequent as Hib (15 cases, 2 %). No Hic and one Hid were isolated. Among the analyzed cases, the age group most affected was > 40 years (638 cases; 88 % of all cases). In addition, a significant percentage of cases (39 cases; 5 %) was found in children aged <5 years.
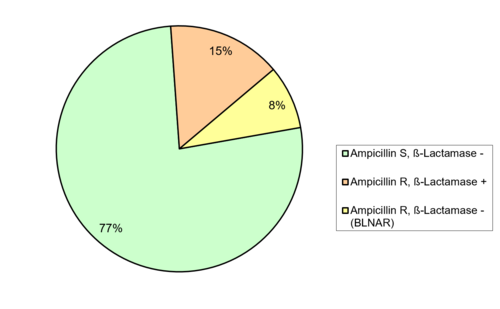
The NRZMHi analyzed the frequency of ampicillin resistance using gradient agar diffusion tests. One hundred and seventy three (23 %) were ampicillin resistant (MIC > 1 µg/ml), of which 109 (15% of all isolates) showed β‑lactamase production. The NRZMHi has tested all isolates for cefotaxime susceptibility. Resistance to cefotaxime was found in 8 isolates (1 %).
2. Serotype distribution of H. influenzae isolates from blood or CSF
3. Age distribution of patients with H. influenzae detected in blood or CSF
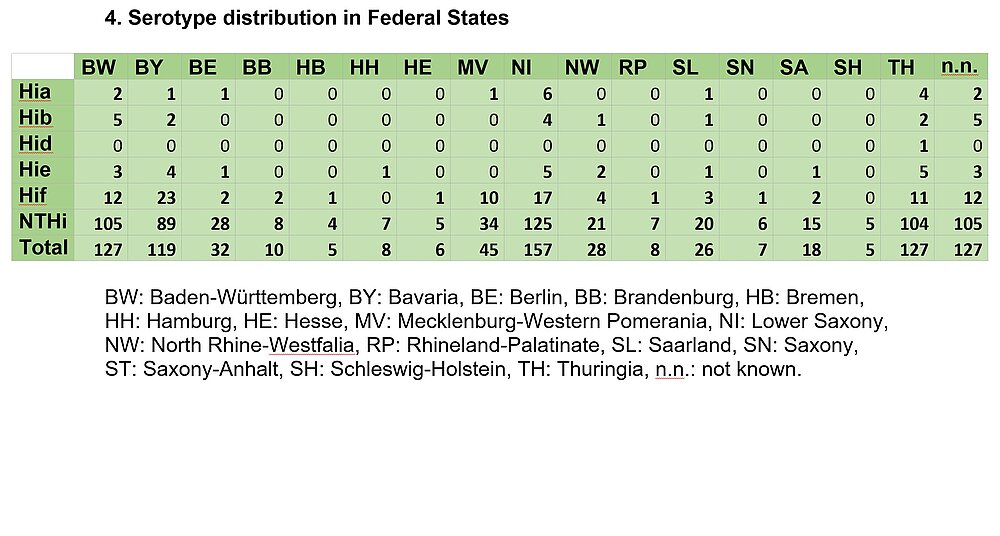
4. Serotype distribution in Federal States
5. Ampicillin resistance in isolates H. influenzae from blood or CSF
7. Publications of the NRZMHi on Haemophilus influenzae:
Original Articles
- Lâm TT, Elias J, Frosch M, Vogel U, Claus H. New diagnostic PCR for Haemophilus influenzae serotype e based on the cap locus of strain ATCC 8142. Int J Med Microbiol. 2011 Feb;301(2):176-9.
- Lâm TT, Frosch M, Claus H, Vogel U. Sequence analysis of the serotype-specific synthesis regions II of Haemophilus influenzae serotypes c and d: evidence for common ancestry of capsule synthesis in Pasteurellaceae and Neisseria meningitidis. Research in Microbiology 2011 Jun;162(5):483-7.
- Lâm, T.T., Claus, H., Elias, J., Frosch, M., Vogel, U., 2015b. Ampicillin resistance of invasive Haemophilus influenzae isolates in Germany 2009-2012.Int J Med Microbiol. 2015 Oct;305(7):748-55.
- Lâm, T.T., Claus, H., Frosch, M., Vogel, U., 2016. Analysis of non-typeable Haemophilus influenzae in invasive disease reveals lack of the capsule locus. Clin Microbiol Infect. 2016 Jan;22(1):63.e7-8
Reviews
- Lâm TT, Claus H, Elias J, Hellenbrand W, Imöhl M, Prelog M, Sing A, van der Linden M, Vogel U. Infections with Pneumococci, Menigococci, H. influenzae and Diphtheria in Germany: the RKI Reference Network for Invasive Bacterial Infections (IBI) at the 5th Würzburg Workshop on Epidemiology, Prevention and Therapy for Invasive Meningococcal Diseases 2010 (Meeting Report). Gesundheitswesen. 2011. DOI: 10.1055/s-0031-1286269.
Disclaimer: the above data were generated with federal funds (RKI). Scientific use is prohibited without prior written consent by KLHi or RKI. Commercial use is strictly prohibited. Inclusion of figures or tables in talks or oral presentations is not allowed.